Anesthesia: Potential for Permanent Neurological Effects
The level of pain experienced by the mother during childbirth is one of the primary concerns for the physician. However, as shown in the peer reviewed
journals below, there is evidence showing the potential for anesthesia to cause not only temporary harm, but also permanent neurological harm as well. This can be observed in the form of in increase in irritability as well as future reductions in IQ (referenced below). Therefore, it is the responsibility of the physician to inform mothers of this potential so decisions can be made accordingly.
Anesthesia effects are not limited to only childbirth, local anesthetics are administered in dentistry being shown to rapidly
cross the placenta. The common local anesthetic lidocaine has been shown to take longer to
clear the fetal circulation than in an adult. The half life for lidocaine in nonpregnant
rats is similar to that for nonpregnant humans, about 2 hours in each. The primary
metabolite of lidocaine, glycinexylidide, is thought to be centrally active and has a half
life of about 10 hours.
Doctors Bowman and Smith have suggested that drugs which
alter central neurotransmitters when administered to the adult may produce irreversible
changes in development of neurotransmitter systems when administered during a sensitive
period in development (5).
In a statement by anesthesia researcher, Dr. Albert R.
Hollenbeck,
(see reference at end of introduction),
"If their hypothesis is correct,
administration of local anesthetics such as lidocaine during a sensitive period in
gestation should be capable of producing enduring changes in offspring behavior, since
they are available to the fetal Central Nervous System, and since they may have effects
upon the central nervous system."
Background on Animal
Anesthesia Studies
Other studies of general inhalation anesthetics have been
reported to cause a wide variety of toxic effects that generates serious concern regarding
potential long lasting effects upon the developing baby. For example, decreases in DNA
content in the bronchial cells of dogs has been reported after exposure to the common
inhalation anesthetic enflurane (Anesthetist 28:120-124, 1979). Abnormal cell
division was induced by enflurane in mammalian and chicken embryo cells (Environmental
Research 12:366-370, 1976). Problems in sperm production in mice have also been found
to occur after exposure to enflurane (Anesthesiology 54:53-56, 1981).
How Common are
Anesthetic Exposures During Pregnancy?
JOURNAL: Child
Psychiatry and Human Development, 16(2):126-134, 1985
In a study originally designed to examine factors in
pregnancy that might relate to cerebral palsy and other forms of damage to the central
nervous system, researchers also gathered information on anesthesia exposure. Information on 50,282 mother-child pairs was collected. Subsequent
analyses showed an overall prenatal exposure rate to local anesthetics to be 11.34% and a
first trimester exposure rate of 5.28% More recent findings reported by Blair et al.,
found in contrast to the first study, more than 20% of normal pregnancies received local
anesthetic agents during pregnancy (does not include delivery exposures which are, of
course, much higher figures), however, the sample size in the Blair study was
notably smaller, leaving open the possibility of sample selection bias.
In an attempt to shed more light on these discrepancies, a
1982 research project was conducted by Dr. Albert Hollenbeck and colleagues at George
Mason University which analyzed 229 low risk mothers of healthy full term deliveries (64%
of the mothers were black, 34% white) to determine the full extent of anesthetic exposure
during pregnancy.
The results of their findings showed 47% of the mothers
(108 women) had visited a dentist during pregnancy and 23% (52 women) received some form
of medication during the visit, usually local anesthesia by injection. In a review of the
mothers’ dental records, lidocaine was the most frequently used anesthetic, followed
by mepivacaine and nitrous oxide.
When analyzing the outcomes of the "anesthetic
exposed" and "not exposed" infants, the researchers found mothers exposed
to anesthetics during the nine months of pregnancy had babies that weighed 279 grams less
at birth. Also of interest, the researchers found that mothers exposed to anesthetics who
also engaged in indoor house painting, had even lower birthweight infants, indoor latex
paints contain the chemicals vinyl acetate and ethylene glycol, and at that time in early
1980’s, indoor wall paints also contained a mercury fungicide which was banned in the
early 1990’s after reports to the EPA of neurological problems in children after
paint exposure.
In conclusion, the researchers stated,
The present findings, in conjunction with the Blair et al. results, are suggestive that
prenatal exposure to anesthetic agents may affect physiological mechanisms which have
behavioral consequences.... Low birth weight could be an indication of disruption in these
metabolic processes (the metabolic process of carbohydrate uptake and protein synthesis).
Previous human observations and considerable animal data suggest that early trimester
anesthetic exposure may result in neonatal behavioral changes."
Dr. Albert R. Hollenbeck, Ph.D. Robert F. Smith, Ph.D. Eleana S Edens,
B.S.
George Mason University, Columbia Hospital for Women
Georgetown University Medical
School
Local Anesthesia During Childbirth
Babies More Irritable & Less Alert
JOURNAL: Science 186: 634-635
(1974)
Abstract Quote:
"Administration of local-regional anesthesia during
normal deliveries was correlated significantly with newborn behaviors as evaluated by the
Brazelton neonatal assessment scale. Three days after birth, infants whose mothers
received local-regional anesthesia were more irritable and motorically less mature than
those infants whose mothers were not medicated."
Babies who were the most alert, the least irritable, and
those who had the most mature motor skills were found to be the ones who were not
exposed to local-regional anesthesia during childbirth, according to research at the National
Institute of Child Health and Human Development in Bethesda, Maryland. The research was
designed to study the possible effects of local-regional anesthetics on behavior
characteristics of infants 3 days of age. Doctors tested 60 first-born, healthy infants
between 48 and 72 hours of age. The children were born to white middle-class women who had
received normal antenatal care and had medically uneventful pregnancies and deliveries.
The most frequently administered analgesic agent was Demerol (meperidine) in conjunction
with the preanesthetics Phenergan (promethazine hydrochloride) or Vistaril (hydroxyzine
pamoate); morphine was given to two women. No women in the study received general
anesthesia. Anesthetic solutions used were lidocaine, tetracaine, mepivacaine, and
bupivicaine. Of the 52 women who received anesthesia, 42 were given spinal (saddle block)
anesthesia, The routes of administration for the other women were pudendal (four),
paracervical (one), epidural (two), both epidural and saddle block (two), and both
pudendal and saddle block (one). Eight women received no anesthesia.
Infants were evaluated by the Brazelton Neonatal Assessment
Scale which tested the following behaviors:
- Alertness: the infant’s responsive to visual and
auditory, animate and inanimate stimuli
- Irritability: the frequency and conditions of state
changes and irritable behaviors
- Motor maturity: the arcs and smoothness of the
baby’s movements, tremulousness, and frequency of startling.
Specific scores on the Brazelton newborn scale showed a 50%
poorer score on irritability measures for the "anesthesia exposed"
group than the "no-anesthesia" group (20.2 versus 13.5). Motor maturity
scores were also found to be 25% lower for the anesthesia exposed babies (21.1 versus
15.1).
According to the research physicians,
"Administration of local-regional anesthesia is
correlated significantly with decreased motor maturity and greater irritability. Jerky
movements in small arcs, startles and tremulous motions, and frequent state changes and
crying were more common in babies of mothers who received anesthesia. Analgesia usage is
significantly related to lower scores on motor maturity.... It is known that anesthetic
agents cross the placenta and enter fetal circulation,. There is no evidence, however,
that these drugs are present in infants later than 1 day after birth. Mepivacaine (a
common local anesthetic) was detected in infants’ blood as late as 24 hours after
birth, and lidocaine, as late as 8 hours after birth.....Whatever the interpretation, it
appears that anesthesia administration during childbirth is significantly related to the
functioning of the newborn child. Local-regional anesthetics although known to produce
severe physiologic reactions in high doses, continue to be considered a safe choice in
standard obstetric procedures. Our data raise questions about the assumption that routine
usage of these anesthetic agents is inconsequential, even for the normal, healthy
infant."
Drs. Kay Standley, A. Bradley Soule III, Stuart A.
Copans and Michael S. Duchowny
Social and Behavioral Sciences Branch,
National Institute of Child Health and Human
Dev., Bethesda, MD
IQ Scores
Lower in 4 Year Old Children
Exposed to Anesthetics During Pregnancy
JOURNAL: Child
Psychiatry and Human Development, 17(1), Fall 1986
Abstract Quote:
"This brief report provides the four year
follow-up on infants prenatally exposed to anesthetics. Fourteen of 39 infants examined at
birth were available for intelligence testing at age four. Results indicate that Peabody
Picture Vocabulary IQ scores are correlated with visual preference testing at birth in
infants exposed to prenatal anesthetics. The mean IQ’s of these infants also differed
from mean IQ’s of unexposed infants at four years. These preliminary data are
suggestive of prenatal anesthetic effects that are persistent and that early infant visual
screening may be predictive of later IQ."
This anesthetic exposure study measured IQ scores in 4 year
old children who were exposed to anesthetic compounds during pregnancy, excluding
anesthetics given at birth. Three standardized intelligence measures were given to each
child by a trained tester who was not aware of the child’s exposure history, (1) the
Peabody Picture Vocabulary Test (PPVT); (2) the vocabulary portion of the Weschler
Preschool Primary Scales of Intelligence; and (3) the picture vocabulary portion of the
Stanford-Binet Intelligence Test.
Of the three tests given, there were no significant
differences found between the anesthesia exposed and non-exposed children on the
vocabulary portion of the Weschler and the picture vocabulary portion of the
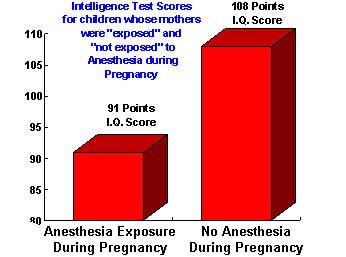
Stanford-Binet tests. However, differences were detected between groups on the Peabody
Picture Vocabulary Test. In fact, over one standard deviation separated the means of the
anesthesia exposed group and the unexposed group. IQ scores on the PPVT averaged 91 for
the anesthetic exposed children and 108 for the unexposed children.
These differences can be seen in the graph at top right.
The one weakness of the study is the small number of
children (14 total) used in the evaluation. Eight were male and six were female. However,
the researchers concluded their report by stating,
"While the few subjects available at four years
cloud definitive conclusions about prenatal drug exposure, the significant findings speak
to the potential strength of drug effects on human behavior. These preliminary results
again clearly suggest the need for a well-controlled extensive human study of prenatal
anesthetic exposure."
Dr. Albert Hollenbeck, Ph.D. Leslie A. Grout, B.S., Dr.
Robert F. Smith, Ph.D.
George Mason University
Columbia Hospital for Women and Georgetown University Medical
School
DNA Damage & Common Anesthesia "Enflurane"
JOURNAL: Environmental
Research, 59:476-484 (1992)
Damage to the DNA molecule within the cells (the DNA
molecule holds our 100,000 genes) has been found to occur after exposure to the common
inhalation anesthetic compound enflurane. Researchers at the Department of Physiological
Chemistry, University of Mainz, Germany, found that exposure to enflurane at levels of
0.2% volume resulted in DNA damage to the immune systems of test animals, The damage was
comparable to damage after X-radiation levels of 0.1 Gy.
The researchers stated in conclusion,
"DNA single-strand breaks are common
phenomena and indicate genotoxic effects even before DNA repair begins. The detection of
DNA single-strand breaks is an instantaneous indication of genotoxicity. However, DNA
repair is not always perfect and because of these deficits in DNA repair mechanisms, one
can draw conclusions from the presence of DNA single-strand breaks about the rate of
possible irreversible DNA damage. For patients with genetic defects in DNA repair, i.e.,
in patients with xeroderma pigmentosum, anesthesia with enflurane may induce irreversible
DNA damage. Determination of DNA damage in cultured cells of these patients before
anesthesia is particularly important in evaluating potential side effects of anesthesia
especially of repeated anesthesia."
The authors also stated that enflurane also affects
mechanisms of mitosis (cell division) and synthesis of nucleic acids (the actual making of
genes and DNA). This potential would, therefore, also generate concern for possible harm
to the rapid neurological development of the growing embryo and fetus.
Drs. Manfred Reitz, Kunti DasGupta, Ludwig Brandt
Department of Physiological Chemistry and Clinics for Anesthesiology
University of
Mainz, Germany
For information on other environmental
circumstances
shown to damage brain growth during
pregnancy - visit
chem-tox.com/pregnancy/learning_disabilities
Additional References
Developmental Child Neurology 26 or 28:476-, 1984 |
